What is it like to have the most important bone in your body split in half, exposing, arguably the most important organs in your body, the heart, and lungs? In two words, frightening and painful! Having been in the Cardio Vascular marketplace for over 30 years, I had seen many of these procedures up close and personal as a part of my job selling and installing heart valves, oxygenators pumps, etc. However, my duties never required me to spend time with patients post sternotomy to get an appreciation for the recovery process. Therefore, when it quite suddenly came to my turn to undergo this procedure, I was almost totally unprepared for what the recovery process would entail, both physically and mentally.
After being told after my angiogram that I needed to undergo surgery immediately for a quadruple bypass, I was totally shocked as I was expecting that I would "probably need a stent at most", in the words of my cardiologist. The good news is that I knew all the key players in the Operating Room including the surgeon, perfusionists and anesthesiologist. Further, they were using virtually all the brand name devices and pieces of equipment I had been marketing for years. Therefore, after being given a sedative I engaged in some light banter and joking with the team, becoming both relaxed and comfortable.
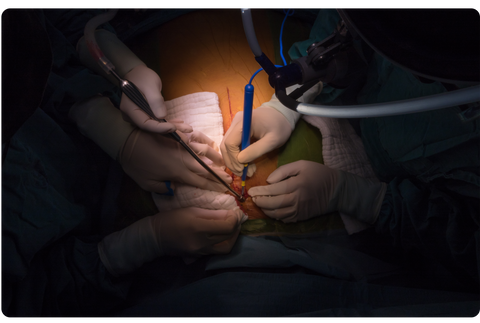 Upon waking many hours later, I felt like the steamroller that I had been dreaming about had indeed run over me! The feeling was immediate weakness, helplessness combined with a total inability to get comfortable as all positions hurt, especially when I tried to move and even breathe normally. I felt totally paralyzed and afraid to move both because of the pain and, as not to disturb the healing process ie. not pull myself apart! To make things worse almost immediately upon waking the nurses wanted me to breathe deeply many times a day, sit up, and begin walking. During this process, the only covering on my sternotomy was a light bandage. They also gave me a heart pillow which hurt like the dickens when pressed against my sternum as instructed during coughing or deep breathing. Of course, I knew that my sternum had been wired together but with every breath or movement I could feel those two sternal halves rubbing, yes grinding against each other. This was not only quite painful but very anxiety-producing, creating fears that the wires may not hold if I move too suddenly, or forcefully and god forbid that I ever had a coughing spasm or worse yet, have to sneeze! In fact, I had been pre-warned by a former patient who said his first sneeze was the scariest and most painful moment he experienced. Thus, I completely stifled sneezing for a full three weeks! When I finally did sneeze it was still very frightening and painful. Unfortunately, I had heard accounts of patients actually coughing and/or sneezing right through their sternotomy wires so naturally anxiety was high.
Upon waking many hours later, I felt like the steamroller that I had been dreaming about had indeed run over me! The feeling was immediate weakness, helplessness combined with a total inability to get comfortable as all positions hurt, especially when I tried to move and even breathe normally. I felt totally paralyzed and afraid to move both because of the pain and, as not to disturb the healing process ie. not pull myself apart! To make things worse almost immediately upon waking the nurses wanted me to breathe deeply many times a day, sit up, and begin walking. During this process, the only covering on my sternotomy was a light bandage. They also gave me a heart pillow which hurt like the dickens when pressed against my sternum as instructed during coughing or deep breathing. Of course, I knew that my sternum had been wired together but with every breath or movement I could feel those two sternal halves rubbing, yes grinding against each other. This was not only quite painful but very anxiety-producing, creating fears that the wires may not hold if I move too suddenly, or forcefully and god forbid that I ever had a coughing spasm or worse yet, have to sneeze! In fact, I had been pre-warned by a former patient who said his first sneeze was the scariest and most painful moment he experienced. Thus, I completely stifled sneezing for a full three weeks! When I finally did sneeze it was still very frightening and painful. Unfortunately, I had heard accounts of patients actually coughing and/or sneezing right through their sternotomy wires so naturally anxiety was high.
So what is the bottom line? I know that if I had the availability of Qualiteam's QualiBreath, that there would have been a tremendous reduction in the amount of pain and soreness which I felt and the accompanying anxiety. This certainly would have dramatically decreased my need for the opioids as well as enabled me to be more mobile, less anxious and I am sure, hastened my overall recovery, thus speeding my feeling of well being and normalcy.
You can take it from me, if and when I have to have a repeat sternotomy or any other major surgical procedure, the FIRST thing I am going to ensure is that I have a Qualiteam Wound Support Product!
Al Seck

1 comment
Apr 19, 2020 • Posted by rick shockley
A true life experience describing the efficacy and need of the Qualibreath.
Leave a comment: