In typical fashion the surgeon will bring the breast bone back together using wire. This helps the stability of the bone during the recovery process. Around 6-8 weeks are expected for the bone to heal properly (without any complications), while recovery from an open heart is variable from person to person.
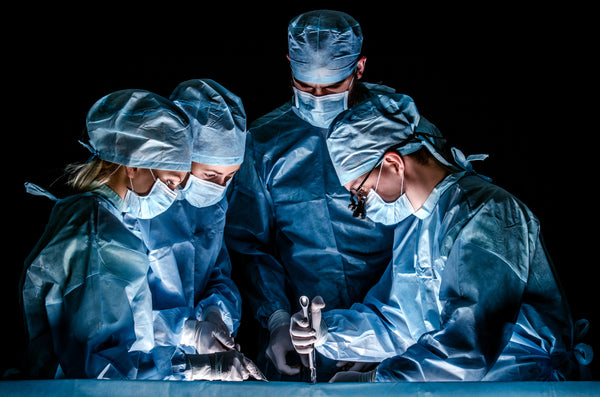
Following surgery, your physician may ask to you complete a cardiac rehab program and/or implement sternal precautions, both can vary from physician to physician, as well as facility to facility.
You may encounter many faces during your hospitalization. All are working together to get you back to your normal daily activities as soon as possible. The team can consist of physical and occupational therapy, dietary, social work, cardiac rehab specialist, pharmacists, and respiratory therapists. While it may seem overwhelming, they are all there to benefit you.

Following your surgery, you will be admitted to the ICU. Here you will be given time to awaken from anesthesia, and have the breathing tube from surgery removed. Here your vital signs will be closely monitored, and family can have short visits. When you are deemed stable from the doctor’s standpoint, you will be moved to the step-down or general surgery unit to begin your recovery. Currently, research has shown getting out of bed and becoming mobile while adhering to sternal precautions sooner, can significantly decrease postoperative complications. Some of these would include sternal wound infections, pulmonary complications, and persistent (chronic) pain.
What are sternal precautions you may ask?
Sternal precautions are designed to help prevent separation of the breast bone during the healing process. While these can vary from doctor to doctor, most common can be found in the list below.
- No lifting anything weighing more than 8-10 pounds
- No Raising arms or reaching over your head
- No Reaching behind your back with arms
- Stopping the activity if you hear any clicking/popping in your chest
- Avoid pushing or pulling with your arms
- Minimizing stair rail use
Immediately after surgery, you may often find it painful to sit up from a lying position or to stand up from a chair. Your physical therapist may show you alternative methods to assist you with this to minimize pain and protect your incision. It may be recommended to use an external chest support device to ease pain associated with movement, coughing, and sneezing.
A system that provides both a constant circumferential chest support, and additional on-demand chest surrounding support, can help minimize the risk of the complications as described above. In the diagram below you can see a variety of ways to move safely using the latest research philosophy of “Keeping it in the tube”.
The left side of the Keep, Your Move in the Tube graphic contains visual tips for staying “in the tube” while performing commonly recommended techniques for getting out of bed. Examples are: side-lying and placing one or both hands in front of the body, leaning forward, and pushing up to a sitting position; leg rolling; and/or the elbow method (leg rolling and counterweighting).

As you can see on the right side of the graphics upper arms and elbows are kept close to the body while performing activities, as to not put a strain on your incision area. You will find you begin to use more of your leg muscles than arm muscles, you may even experience soreness in your legs from this.
By learning and practicing these techniques, they can be applied to progress your recovery. You may have set goals of walking, activities of daily living (dressing, grooming, etc) to be considered for discharge from the hospital.
Discharge from the hospital will be dictated by many factors determined by your doctor. Examples of criteria for hospital discharge may include: normal heart rhythm, absence of wound infection, normal routine blood tests, satisfactory chest X-ray, and full mobility. Toward the end of your hospital stay, the therapy team's assessment of mobility status is a major determinant of whether a patient needs rehabilitative care after being discharged. Instead of going home with a doctor’s referral for outpatient cardiac rehabilitation, they may suggest you for an inpatient rehabilitation facility for a short time.
Although it may be difficult to start a cardiac rehabilitation program when you're not feeling well, it can benefit you in the long run. Cardiac rehabilitation can guide you through fear and anxiety as you return to an active lifestyle with more motivation and energy to do the things you enjoy. Here you will continue to build strength and endurance to prepare to go back home. It will also guide you when you are ready to resume such household responsibilities such as laundry, washing dishes, cooking, light cleaning, and even driving yourself.
Remember during your recovery to using common sense is the best way to keep yourself from overdoing it. Cardiac rehab is very beneficial to restore your health and guide you on how to change lifestyle habits to help prevent future heart problems or conditions.
“According to studies, people who go to cardiac rehab have up to 30 percent fewer fatal heart events, and are 25 percent less likely to die compared to people getting standard therapy alone.”

- lifting weights -- hand weights, free weights, or weight machines
- using a wall pulley
- using elastic bands or body weight
Generally, these activities are recommended 2-4 times a week, with each session lasting from 30-45 minutes as tolerated. Always discuss with your doctor prior to starting an exercise program following heart surgery.
Depression and anxiety are common among people with heart disease or who’ve had a heart attack or heart surgery. There many resources available to help prevent feelings of depression and anxiety located both in the communities and online. As responsibilities may have shifted at home, staying in communication with those closest to you, and verbalizing feelings can alleviate symptoms. Many people find that keeping some sort of routine is very helpful for staying positive during recovery, too. Routines can include whatever keeps your spirits up, provided you have your healthcare providers’ okay.
Sample daily routine:
- Try to get at least 8 hours of sleep each night. Go to bed at the same time each night.
- Wake up and shower each morning at approximately the same time.
- Weigh yourself daily.
- Get dressed in regular daytime clothes. This will make you feel more like being active.
- Eat breakfast.
- Take your medication.
- Plan your day during breakfast to help you from getting too tired.
- Follow the walking plan provided by your physical therapist.
- Avoid prolonged naps in the daytime—they may prevent you from sleeping at night.
Great support groups with those who have had similar procedures can be found, here are a few links to reach out.
https://www.womenheart.org/find-support/
https://supportnetwork.heart.org/
Incorporating social and exercise activities can also help alleviate symptoms of depression. If you feel you are not able to control the feelings of depression or anxiety, it is recommended to talk to your doctor for options such as medications or behavioral therapy counseling.
As you make great strides in your recovery, take time to celebrate little victories. Maybe you walked for 30 minutes and didn’t get short of breath or stopped to take a break, congratulate yourself. Maybe your heart doctor gave you praise for how well you have done during your recovery, treat yourself or pamper yourself with something you enjoy. Heart surgery can fix immediate concerns of the heart, however, long term recovery involves fighting any potential risk factors (i.e. family history, dietary and exercise habits) in an ongoing fashion. Healthy lifestyle changes make a big impact on your future health and preventing complications down the road. If you stick with what you learn in your cardiac rehab program, you may soon find you are feeling even better than before you had a heart condition or had heart surgery.
References:
- Cahalin, L et al. Sternal precautions: is it time for change? Precautions versus restrictions - a review of literature and recommendations for revision. Cardiopulm Phys Ther J; 22(1): 2011: 5-15.
- http://ctsurgerypatients.org/pre-post-operative-care/after-heart-surgery
- Balachandran S, Lee A, Royse A, Denehy L, El-Ansary D. Upper limb exercise prescription following cardiac surgery via median sternotomy: a web survey. J Cardiopulm Rehabil Prev. 2014;34(6):390–5.
- https://www.cardiosmart.org/Heart-Basics/Understanding-Cardiac-Rehabilitation
- Baylor Heart and Vascular Hospital (Adams, J et al. An Alternative Approach to prescribing sternal precautions after median sternotomy. Proc (Bayl Univ Med Cent). 2016 Jan;29(1):97-100.

8 comments
Mar 21, 2025 • Posted by aldo juan fernandez
me hicieron dos vay pas en el corazon me camviaron dos arterias en el sanatorio santa fe iden provincia argentina llegue con un dolor en el pecho me hucieron el estudio y detectaron que tenia las arterias tapadas el 31 de enero de 2.023 me operaron no senti jamas un dolor a los 5 dias me dieron de alta porque tengo familiares en esa ciudad y el 14 de febrero me permitieron viajar a mi ciudad 100 kmts lo unico que siento segun el movimiento es como que sede algo adentro del pecho sin dolor no me levanto solo me ayudan y me siento tomando de los brazos y me levanto de la silla usando nada mas que las piernas me gustaria saver si es normal lo del pecho gracias y un gran agradecimiento al sanatorio dsanta fe y a todo el personal el cirujano e el dr kabermater
Feb 21, 2023 • Posted by Gracias...tenia dudas en cuanto a los ejercicios que podía hacer los límites para ellos...ahora me pregunto cuanto tarda en sanar las arterias añadidas xq aun se siente ardor a los 3 meses de la operación.....🤔
Gracias…tenia dudas en cuanto a los ejercicios que podía hacer, los límites para ellos…ahora me pregunto cuanto tarda en sanar las arterias añadidas xq aun se siente ardor a los 3 meses de la operación….y saber tambiéncuantotarda en desincharse el pié de la pierna herida….🤔
Jan 19, 2023 • Posted by Francy Angel
Muy buenas recomendaciones, me gustan los consejos, pues después de la cirugía, uno queda con muchas incertidumbres. Muchas gracias
Jan 19, 2023 • Posted by BERRADJ
Un grand MERCI .
Aug 18, 2022 • Posted by RonL
5 weeks post open heart surgery. Aortic valve and partial aorta replacement. Almost no pain from the actual surgery. Incision healed quickly and sternum appears to be healing. A little odd feeling in muscle in left chest when I move right arm – odd. Still working on getting appetite back and getting enough sleep. Walking a little over a mile each day. Tiredness was my biggest issue. Discovered the valve issue 5 years ago and had no symptoms. Still had no symptom right up to surgery but dr advised I do the surgery while there were no other health issues at 72. So it seemed odd to go into surgery when I still felt fine. But St Lukes in Kansas City did a great job and hopefully I will not need any further heart repairs - ever !!!!
Aug 03, 2022 • Posted by Ken Martin
Cardiac Rehab has been huge for me, but I did not realize how dramatic the stats are in saving and extending life. Do it! Personally, I am itching to get back on the golf course. As well as my rehab is going, I’ll be back to butchering courses in no time.
May 07, 2021 • Posted by Mark Fischer
Excellent advice! My will to do more activities has indeed been helpful!….however the practical advice in this article is so true…don’t overdue physical activity! Listen to your body & mind & slow down as you slowly build up your body strength!
Nov 03, 2020 • Posted by Mervyn Kirkpatrick
Really good advise and was worth reading thank you
Leave a comment: